Catastrophic Disaster Response Staff Officer's Handbook
Handbook 06-08
May 2006
Casualty Considerations, Tactics, Techniques, and Procedures
Appendix B
The delivery of public health and medical support falls under emergency support function (ESF) #8 of the National Response Plan (NRP). The Department of Health and Human Services (DHHS) serves as the primary agency for these functions; nevertheless, this ESF is one in which the military is likely to be involved. When required, the Joint Regional Medical Planner Office (JRMPO) of Northern Command (NORTHCOM) and the defense coordinating officer (DCO) coordinate these services. The joint task force’s (JTF) medical planning staff must be in close contact with these offices as they develop their operational plans. However, there are several acute situations that the JTF will likely encounter before it has the opportunity to coordinate with these offices. These include mass casualty operations, contaminated casualties, and mental health casualties. Also, JTF planners should be aware of National Disaster Medical System (NDMS), a Federal Emergency Management Agency (FEMA) organization responsible for supporting and coordinating the federal medical response to disasters.
Mass Casualty (MASCAL) Operations
Disaster situations, whether the result of natural or man-made incidents, can quickly produce a large number of casualties across a widespread geographic area. This may, in turn, overwhelm the existing health care system and produce either a local or area-wide MASCAL situation. MASCALs are inherently difficult to control, especially across large areas, and contain several major obstacles to the delivery of health care which the JTF must plan for and overcome. These obstacles include:
- Inappropriate care distribution. Often the first casualties to present for care are the least injured, who then consume all available resources, leaving the most injured without access to life-saving care. To ensure that medical resources are appropriately allocated across the affected area, care delivery must be prioritized at both the local level and area-wide.
- Unequal distribution of casualties. Casualties tend to concentrate locally and then present to the nearest health facility. This may overwhelm local facilities, while other facilities in the area are underused. A variation of this pattern is when casualties take themselves to the “preferred” or “better” hospitals, while avoiding all other, closer facilities.
- Non-Emergency Medical System (EMS) responders. EMS is the usual route of entry into the health care system for casualties. In MASCALs, casualties access the system through non-EMS entry points (for example: private means, police transport, and search and rescue [SAR]). This results in multiple, uncontrolled demands for health care and concentrates the demands at non-typical locations (i.e., at the SAR delivery point, as opposed to the hospital). Also, non-local responders arrive to help but are not familiar with the local health system, adding to the overall confusion.
- Lack of inter-organizational planning. During major disasters, multiple organizations are involved from both within and outside the local area. These may include local, state, and military personnel; public health organizations, non-governmental organizations, and charitable organizations; and private citizens, to name a few. The actions of these groups tend to be uncoordinated, with little to no inter-organizational communication.
- Lack of proper needs-assessment. The acute demand for care often results in a rapid deployment of resources to the most critical and closest casualties, without an overall assessment of need. This “ready, fire, aim” approach leads to a “wrong help, at the wrong time, to the wrong people” situation. Some areas will receive an over-abundance of aid, while others may be completely neglected.
Techniques and procedures to overcome obstacles to care
- Coordinate all missions through the JRMPO, and coordinate with DHHS and all other medical assets in the area.
- Centralize command and control of all military health assets that enter the area.
- Institute a systematic plan for allocation of medical care at ground zero and across the area.
- Ensure coordinated and controlled delivery of casualties located by SAR into the established triage system.
- Coordinate with law enforcement to maintain crowd and traffic control.
- Communicate with local hospitals to determine capacities and capabilities, in order to properly direct casualty flow from ground zero to higher levels of care.
Triage
The key to managing MASCAL situations is triage. Triage is the process of sorting casualties based on the severity of injury and assigning priorities of care and evacuation in a situation with limited resources. The goal is to provide the greatest good for the greatest number of casualties. Medical providers, at all levels of care, must institute a uniformed system to classify casualties and assign treatment priorities..
Triage categories. Triage categories were originally developed for MASCAL management in combat environments. Most military medical personnel are familiar with this system. The same principles apply to the civilian disaster setting, with the major differences being primarily terminology and priority assignment. Table A1-1 depicts triage categories used in combat and natural disasters.
Triage Category: Combat Setting |
Triage Category: Civilian Setting |
Category Description |
Immediate |
Critical |
This group includes those who require lifesaving surgery. The surgical procedures in this category should not be time consuming and should concern only those patients with high chances of survival. |
Delayed |
Urgent |
This group includes casualties who are badly in need of time-consuming surgery, but whose general condition permits delay in surgical treatment without unduly endangering life. Sustaining treatment will be required. |
Minimal |
Minor |
These casualties have relatively minor injuries and can effectively care for themselves or helped by non-medical personnel. Care can be delayed for hours to days. |
Expectant |
Catastrophic |
Casualties in this category have wounds that are so extensive that even if they were the sole casualty and had the benefit of optimal medical resource application, their survival would be unlikely. |
Table A2-1. Triage categories, combat vs. civilian casualties
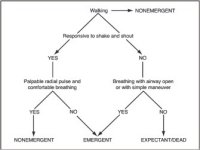
Assigning triage categories. Medical personnel must rapidly assess casualties and assign triage categories. A systematic process should be in place to ensure proper identification occurs. A simple algorithm is suggested in Figure A1-1 to assist with this process.
Treatment priorities. When assigning treatment priorities, the first to receive care are those in most critical need (where there is an expectation that an intervention will prevent loss of life, limb, and/or eyesight) with minimal expenditure of time, personnel, and/or other resources.
In the combat setting, triage principles dictate treating casualties in the “expectant” category after all other wounded; thus “expectant” casualties have a high likelihood of dying. Civilian medical personnel, especially in the United States, view this as an unreasonable approach. It is unlikely that resources would be so constrained such that the seriously wounded should have care delayed for any significant amount of time. It is unreasonable to expect rescuers to “condemn” expectant casualties when not in a tactical combat environment.
Table A2-2 outlines treatment priorities for the different triage categories in the combat and civilian settings.
PRIORITY |
COMBAT CASUALTIES |
CIVILIAN CASUALTIES |
1st |
IMMEDIATE |
CRITICAL |
2nd |
DELAYED |
CATASTROPHIC |
3rd |
MINIMAL |
URGENT |
4th |
EXPECTANT |
MINOR |
Table AB-2. Treatment priorities in a combat vs. civilian MASCAL setting
Management and treatment
Every medical unit or facility that responds to a disaster situation requires a MASCAL plan appropriate to their unique operational needs and situation. However, there are several characteristics that are consistent for all MASCAL operations:
- Triage area. All casualties should flow through a single triage area. This area should be close to the receiving area (landing zone [LZ], ground routes, decontamination site), have one-way flow, and have clearly marked routes to the treatment areas.
- Triage officer (TO). Ideally the TO is a surgeon, but must be a person with clinical experience in evaluating casualties. The TO performs a rapid evaluation of every casualty, assigns them an appropriate category, and directs them to the proper treatment area. The TO is assisted by personnel dedicated to identifying, tagging, and recording triage assignments and disposition.
- Immediate treatment area. This area is set up close to and with direct access to the triage area and is composed of the staff and supplies necessary to administer immediate, life-saving aid.
- Non-immediate treatment area. All minor and delayed injuries are directed here. This area is staffed and supplied to treat all non-immediate injuries and to hold casualties awaiting evacuation to a higher level of care (i.e., a hospital).
- Morgue. This area must be set aside, climate controlled (if possible), and secured from view and interference.
Techniques and procedures for MASCAL and triage
- Ensure traffic flow is well marked so all casualties enter the triage area at one location.
- No significant treatment should occur in the triage area. Casualties are sent to the appropriate treatment area for interventions.
- An administrative recorder should walk with the TO to properly document all casualties in a log and use an indelible marker on the casualty’s forehead to mark his triage category.
- Post an administrative person at the entry of the treatment areas to document and regulate casualty flow.
- Dedicate someone to re-triage casualties as they enter each treatment area.
- Have as many non-medical augmentees as possible available to assist with casualty transport (i.e., litter bearers).
- Shift resources from the triage and emergent area to the non-emergent areas as the casualty flow lessens.
- Ensure proper rest cycles for personnel, especially if operations continue beyond 24 hours.
- Be prepared to divert casualties to another facility as resources are exhausted or overwhelmed.
For further, more detailed information on triage and MASCAL, see:
- Emergency War Surgery, 3rd US Revision, 2004, at www.bordeninstitue.army.mil
- Disaster Response: Principles of Preparation and Coordination; Erik Auf der Heide; 1989, at http://orgmail2.coe-dmha.org/dr/index.htm
Contaminated Casualties
During disaster events, casualties may become contaminated by either a chemical, biological, radiological, nuclear, high-yield-explosive (CBRNE) attack or from exposure to hazardous industrial waste (e.g., sewage, oil spills). In these instances, casualties must be decontaminated before entering any treatment facility; otherwise the treatment facility itself will become contaminated. First responders will decontaminate and treat the majority of these casualties in the initial hours after the event.. However, if recovery operations continue in a contaminated area, there will be an ongoing need to decontaminate and treat casualties. The joint task force's (JTF) medical assets will become involved in these situations.
Radiological (i.e., a dirty bomb) and biological weapons generally only impact the individual casualty, and this type of contamination is unlikely to spread to others. Biological and radiological contamination is usually eliminated with soap and water, and is of little tactical significance to casualty care. Likewise, industrial toxins and wastes are also easily cleaned by simple washing procedures. These types of contamination can be handled by routing casualties through washing and monitoring stations prior to them entering a treatment facility. Chemical casualties, with their potential to contaminate other personnel and facilities, require detailed decontamination plans.
Casualty decontamination is labor-intensive and requires augmentation personnel and additional, or specialized, equipment. It slows the process of casualty evaluation and treatment and is physically demanding of medical and rescue personnel. These negative impacts can be minimized with proactive planning.
Responders
Due to the abrupt, immediate nature of a CBRNE event, the initial responders will be local hazardous material (HAZMAT) units and state National Guard units. The National Guard has established weapons of mass destruction (WMD) civil support teams (WMD-CST), and chemical, biological, radiological, nuclear, or high-yield-explosive enhanced response force packages (CERFP). The WMD-CST mission is to support local and state authorities at domestic CBRNE events, identify agents and assess consequences, and advise local authorities on response measures and requests for military assistance. The primary missions of the CERFPs are casualty decontamination and triage and SAR in contaminated environments. In all likelihood these units will be in place and operational by the time federal military units arrive on the scene of a CBRNE attack. Therefore, these units act as an “advance party” for other military units.
The specific technical aspects of casualty decontamination exceed the scope of this handbook, but the following general concepts apply to all operations:
- Establishing the decontamination site. The casualty decontamination site should be as near to the medical facilities as safety allows, but not so near that it risks contaminating the treatment facility. When establishing the decontamination site, planners must consider:
- Wind direction and speed. While the patient decontamination site will be established in a “clean” location, the arrival of casualties and the initiation of decontamination procedures will create chemical vapor and liquid hazards. Wind direction and speed must be constantly monitored to ensure that all clean areas (i.e., clean treatment areas, the rest of the medical unit, other units or personnel in the area, etc.) are not contaminated. If the wind direction shifts more than 30 degrees, the decontamination site may need to be moved.
- Access and movement control. Access to the site must be controlled; otherwise there is the possibility that “dirty” casualties and equipment will contaminate the “clean” areas. There should be one entry point and controlled and limited areas of intersection between the clean and dirty zones. All personnel and equipment must remain in a “dirty” zone until decontaminated.
- Personnel and equipment. Once personnel and equipment become contaminated, they remain “dirty” until decontaminated. Personnel can and should continue to treat patients and use equipment in the contaminated area for as long as possible. However, operating in this environment is physically demanding and will require additional personnel and the institution of strict work-rest cycles.
Key Elements of Casualty Decontamination
The management of contaminated casualties is complicated in that they must be evaluated and, possibly treated and evacuated, while still contaminated.
- Dirty triage. Casualties must be triaged upon arrival to the treatment facility while still contaminated. The determination made at this point is, not only the immediacy of treatment based on injury, but whether the casualty needs to be treated before or after decontamination.
- Dirty treatment. There may be casualties who require immediate treatment before decontamination. At the decontamination site, there must be a treatment area, with supplies and personnel, established within the “dirty” area.
- Dirty evacuation. Casualties may need to be evacuated while still contaminated. This may be because the patient is minimally injured and does not need decontamination or treatment at the local treatment facility. This could also be because the patient has been stabilized while contaminated, needs further treatment, and it is a better use of resources to evacuate to another facility for decontamination and further treatment. In these cases, there must dedicated evacuation lanes and equipment that will remain contaminated until the end of operations.
Techniques and procedures for contaminated casualty care
- All deploying medical units must prepare to operate in a contaminated environment.
- Establish contact with any WMD-CST and CERFPs present prior to entering the area. This will allow for a smooth handoff of responsibilities and ongoing support.
- Clearly designate clean versus contaminated areas in the area of operations.
- Develop clean and dirty triage and treatment sites and evacuation lanes.
- Only casualties requiring treatment at the medical facility should be decontaminated at the facility. All others should be evacuated to other decontamination facilities.
- Plan to increase the number of personnel at the treatment site due to increased personnel demands in the “dirty” areas.
- Pre-position traffic control points and guards to maintain access control to the treatment site.
- Carefully monitor wind direction (i.e,. stakes with streamers), and have plans in place to shift the decontamination and treatment sites, if needed.
For further information on the specific details of casualty decontamination, see:
- “Field Management of Chemical Casualties Handbook” Second edition, July 2000, Chemical Casualty Care Division, U.S. Army Medical Research Institute of Chemical Defense (USAMRICD). http://chemdef.apgea.army.mil
Mental Health Casualties
Disaster incidents produce strong and unpleasant emotional and physical responses in both victims and rescuers. Leaders must proactively institute preventative measures, and apply appropriate psychological first aid when indicated. The symptoms of psychological stress that rescuers and victims may experience include: confusion; fear and anxiety; hopelessness, helplessness, or sleeplessness; anger; grief, guilt, or shock; aggressiveness or mistrustfulness; loss of confidence; physical pain; or over-dedication to one’s task.
One particularly stressful activity is the handling of human remains. Working around human remains may produce feelings of horror, disgust, anger, or guilt, to name a few. Many feel very strong emotions when confronted with the remains of children or when the victims remind them of loved ones.
The goal of psychological first aid is to mollify the range of emotions and physical responses experienced by personnel exposed to a disaster. The main tenets of care are to create and sustain an environment of safety, calm, connectedness to others; self-efficacy; and hope.
Techniques and procedures for psychological first aid:
- Provide basic needs for food, shelter, and health care.
- Listen to peoples’ stories.
- Keep families together.
- Provide frequent, clear, updated information to victims concerning the disaster itself, the status of relief efforts, and where and how to acquire assistance.
- Help maintain connection with friends and family. Provide responders with regular communication with family members back home.
- Be aware of the stress levels of those around you.
- Provide responders with a rest area for sleep, hygiene, and food that is separate from the public and media.
- Insist on proper sleep, nutrition, and exercise among responders.
- Do NOT force people to share stories.
- Do NOT give simple, generalized reassurances (e.g.,“everything will be ok.).
- Do NOT tell people how they should feel, or “why” things happened to them.
- Do NOT make promises you cannot keep.
- Do NOT criticize current relief efforts in front of those needing help.
Techniques and procedures for psychological first aid during the handling of human remains:
- Remember the greater purpose of your work.
- Wear protective clothing, take frequent breaks, and maintain hygiene, hydration, and rest when not working.
- Talk with others around you and listen as well.
- Humor relieves stress as long as it is not too personal or inappropriate.
- Limit exposure to bodies as much as possible.
- Breath through your mouth to avoid smells.
- Do not focus on individual victims.
- Get teams together for mutual support and encouragement.
- Provide opportunities for voluntary, formal debriefings
National Disaster Medical System (NDMS)
The NDMS is a federally coordinated system that augments the nation’s medical response capability. The overall purpose of the NDMS is to establish a single integrated national medical response capability for assisting state and local authorities in dealing with the medical effects of major peacetime disasters. The NDMS may be activated for:
- Natural disasters
- Technological disasters
- Major transportation accidents
- Acts of terrorism including WMD events
Its mission is to design, develop, and maintain a national capability to deliver medical care to the victims and responders of a domestic disaster. NDMS provides medical care at a disaster site, in transit from the impacted area, and at participating definitive care facilities.
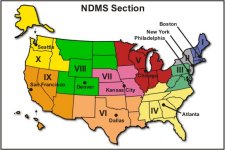
Regional offices for NDMS
Region |
Region |
||
1 |
99 High Street, 5th Floor |
6 |
800 North Loop 288 |
2 |
26 Federal Plaza, 13th Floor |
7 |
2323 Grand Boulevard, |
3 |
One Independence Mall, |
8 |
Denver Federal Center |
National Capital Region |
500 C Street, SW |
9 |
50 United Nations Plaza, |
4 |
3003 Chamblee-Tucker Road |
10 |
130 228th Street, SW |
5 |
536 S. Clark St. 6th Floor |
National Office |
Department of Homeland Security |
Under the NDMS are several unique medical teams:
- Federal Coordination Centers (FCC )
- Disaster Mortuary Operational Response Team (DMORT)
- Disaster Medical Assistance Team (DMAT)
- Veterinarian Medical Assistance Team (VMAT)
- National Pharmacy Response Team (NPRT)
- National Nurse Response Team (NNRT)
FCC
FCCs recruit hospitals; maintain local hospital participation in the NDMS; and, during system activation, coordinate the reception and distribution of patients being evacuated from the disaster area.
In most cases, patients are evacuated out of the disaster area by the Department of Defense (DOD) Aeromedical Evacuation System (AES), which is operated by the Global Patient Movement Requirements Center (GPMRC), of the U.S. Transportation Command. In the event of a disaster, the GPMRC is tasked to deploy the Immediate Response Assessment Team (IRAT). The IRAT determines the need for patient evacuation. If there is a need, a mission tasking order is issued to DOD, and FCCs are activated. GPMRC then issues instructions to the FCCs for the reporting of available beds. Simultaneously, patient information is gathered at the disaster site and forwarded to GPMRC through the IRAT. GPMRC determines to which FCCs the patients will be moved based on the victims’ needs, beds available, and transportation availability. GPMRC coordinates with the IRAT and other deployed DOD transportation elements at the disaster site to ensure smooth air operations.
DMORT
The NDMS provides victim identification and mortuary services. These responsibilities include:
- Temporary morgue facilities
- Victim identification
- Forensic dental pathology
- Forensic anthropology methods
- Processing
- Preparation
- Disposition of remains
DMORTs are responsible for this mission. DMORTs are composed of private citizens, each with a particular field of expertise related to mortuary affairs (e.g., funeral directors, medical examiners, forensic scientists, etc.). During an emergency response, DMORTs work under the guidance of local authorities by providing technical assistance and personnel to recover, identify, and process deceased victims.
In support of the DMORT program, FEMA maintains two Disaster Portable Morgue Units (DPMUs). Both DPMUs are staged at FEMA Logistics Centers, one in Rockville, MD and the other in San Jose, CA. The DPMU is a depository of equipment and supplies for deployment to a disaster site. It contains a complete morgue with designated workstations for each processing element and prepackaged equipment and supplies.
Specific contact information for specific region team leaders can be obtained at the following Website: http://oep-ndms.dhhs.gov/dmort.html
DMAT
A DMAT is a group of professional and para-professional medical personnel (supported by logistical and administrative staff) designed to provide medical care during a disaster or other event. Each team has a sponsoring organization, such as a major medical center, which assembles and coordinates the team. DMATs are designed to be a rapid-response element to supplement local medical care until other federal or contract resources can be mobilized, or the situation is resolved.
DMATs are principally a community resource available to support local, regional, and state requirements. However, as a national resource they can be federalized to provide interstate aid.
DMATs deploy to disaster sites with sufficient supplies and equipment to sustain themselves for up to 72 hours of operations. In mass casualty incidents, their responsibilities include triaging patients, providing medical care at the disaster site, and preparing patients for evacuation. In other types of situations, DMATs provide primary medical care and serve to augment overloaded local health care staffs. In the circumstance where disaster victims are evacuated to a different locale to receive definitive medical care, DMATs may be activated to support patient reception and disposition to hospitals..
To supplement the standard DMATs, there are highly specialized DMATs that deal with specific medical conditions such as crush injuries, burns, and mental health emergencies.
VMAT
The NDMS is directed to provide assistance in assessing the extent of disruption and need for veterinary services following major disasters or emergencies. These responsibilities include:
- Assessing the medical needs of animals
- Medical treatment and stabilization of animals
- Animal disease surveillance
- Zoonotic disease surveillance and public health assessments
- Technical assistance to assure food and water quality
- Hazard mitigation
- Animal decontamination
- Biological and chemical terrorism surveillance
In order to accomplish this mission, veterinary medical assistance teams (VMATs) were developed and are composed of clinical veterinarians, veterinary pathologists, animal health technicians (veterinary technicians), microbiologist/virologists, epidemiologists, toxicologists, and various scientific and support personnel. During an emergency response, VMATs work under the guidance of local authorities by providing technical assistance and veterinary services.
NPRT
NPRTs represent hundreds of pharmacy, pharmacy technicians, and pharmacy students located in each of the ten DHS regions who can be activated to assist in the chemoprophylaxis or the vaccination of hundreds of thousands or even millions of Americans.
NNRT
The National Nurse Response Team is a specialty DMAT that will be used in any scenario requiring hundreds of nurses to assist in chemoprophylaxis, a mass vaccination program, or a scenario that overwhelms the nation’s supply of nurses in responding to a weapon of mass destruction event.
|
NEWSLETTER
|
| Join the GlobalSecurity.org mailing list |
|
|
|