Flu Season
In the northern hemisphere, influenza season runs from October to March, while in the southern hemisphere, the season covers the remaining months, April to September. In the tropics, the influenza virus circulates year round. Its not possible to determine the peak of the influenza season until the flu season is over. Influenza activity typically does not reach its peak in the US until January or February. During the 26 flu seasons prior to 2009, the peak of the influenza season occurred in November one season, December four seasons, January five seasons, February 12 seasons, and March four seasons.
Influenza-like illness (ILI) is defined as a temperature of > 100.0°F (> 37.8°C) and either cough or sore throat in the absence of a known cause. Levels of influenza activity are 1) no activity, 2) sporadic-small numbers of laboratory-confirmed influenza cases or a single influenza outbreak reported but no increase in cases of ILI, 3) local-outbreaks of influenza or increases in ILI cases and recent laboratory-confirmed influenza in a single region of a state, 4) regional-outbreaks of influenza or increases in ILI cases and recent laboratory-confirmed influenza in at least two but less than half the regions of a state, and 5) widespread-outbreaks of influenza or increases in ILI cases and recent laboratory-confirmed influenza in at least half the regions of a state.
Influenza incidence exhibits strong seasonal fluctuations in temperate regions throughout the world, concentrating the mortality and morbidity burden of the disease into a few months each year. Influenza is more likely to spread in the winter than the summer. This may be caused by an increased infectiousness of the disease, an increased susceptibility of people, or an increased number contacts with others that might result in transmitting the infection during the winter. For example, people may spend more time indoors.
The reason that more people catch the flu in the winter appears to be that small seasonal changes in flu transmission at the individual level are greatly amplified as the disease spreads through communities. The underlying cause of seasonal fluctuations in transmission may be too small to measure. Large fluctuations in the number of flu cases between winter and other seasons may be caused by very small changes in the number of people infected by a single infectious person. These small changes in transmission rate are amplified by interactions between the evolving virus and the changing level of immunity that people have to specific strains.
The cause of influenza's seasonality has remained elusive. Studies have failed to establish whether these transmission changes are due to direct effects of temperature and humidity on transmission, to changes in mixing patterns [e.g., school terms or simply more time spent indoors], or to other factors, such as increased viral production under winter conditions. In fact, it may be impossible to establish the underlying cause of seasonality in influenza epidemics, since the large observed oscillations in incidence can be generated by seasonal changes in the transmission rate that are too small to measure. The large oscillations in incidence may be caused by undetectably small seasonal changes in the influenza transmission rate that are amplified by dynamical resonance.
Data can be evaluated quantitatively, and graphic representation of this information, known as epidemic curves (epi-curves), may prove especially useful in this endeavor. These visual representations depict case frequency over time, and are initially used to obtain tentative answers to questions concerning origin, propagation, incidence, prevalence, and likely modes of transmission. The nature of the epidemic curve varies with the pathogen. The frequency curve for most infectious diseases resembles a logarithmic normal curve. Epidemics such as infuenza have distinctive patterns of initiation and spread.

During the 1999-2000 season, influenza type A(H3N2) was the predominant strain circulating in the United States. Influenza activity (virus isolation, morbidity and mortality) peaked between mid-December and mid-January. The percentage of respiratory specimens testing positive for influenza viruses peaked at 33% during mid to late December. During the previous 3 influenza seasons (1996-97, 1997-98, and 1998-99), the peak percentages of respiratory specimens testing positive for influenza viruses ranged from 28% to 34%.

The 2000-01 influenza season was mild in the United States and was the first season since 1995-96 that influenza A(H3N2) viruses did not predominate. The percentage of patient visits for influenza-like illness (ILI) peaked at 4% for 4 consecutive weeks during mid- January and early February. During the previous 3 influenza seasons, the peak percentage of patient visits for ILI ranged between 5% and 7%. On the basis of data from state and territorial epidemiologist reports, influenza activity peaked during late January and early February, when 38 states reported regional or widespread influenza activity. The peak number of states reporting regional or widespread activity during the previous 3 years ranged from 43 to 46.
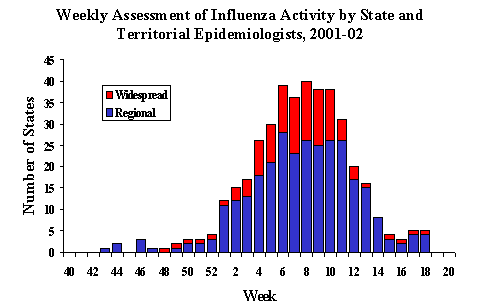
The 2001-02 influenza season was mild to moderate in the United States and influenza A(H3N2) viruses predominated. On the basis of data from state and territorial epidemiologist reports, influenza activity peaked during mid-February, when 40 states reported regional or widespread influenza activity.
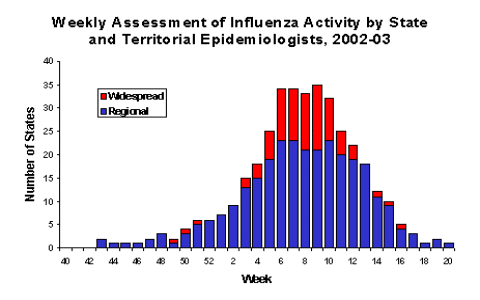
The 2002-03 influenza season was mild in the United States; influenza A(H1) and B viruses circulated widely, and the predominant virus varied by region and time of season. Influenza morbidity peaked during early-to-mid February 2003, and pneumonia and influenza mortality peaked during late February 2003. Human infections with avian influenza A(H5N1) and A(H7N7) viruses were reported in Hong Kong and the Netherlands, respectively. Influenza activity peaked during late February, when 35 states reported regional or widespread influenza activity. The peak number of states reporting regional or widespread activity during the previous 3 years ranged from 38 to 44. During the 2002-03 season, one or more states reported regional influenza activity during 30 consecutive weeks from the week ending October 26, 2002 through the week ending May 17, 2003.
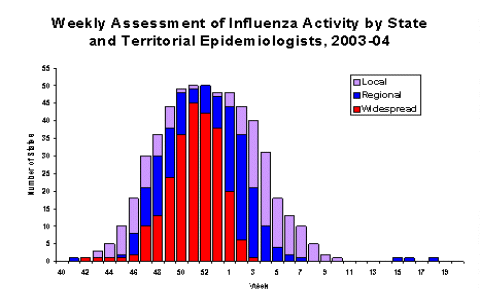
The 2003-04 US influenza season began earlier than most seasons and was moderately severe. The influenza activity level definitions changed for the 2003-04 influenza season to include the addition of a local activity level. In past seasons, this level of activity was most likely reported as regional influenza activity. On the basis of data from state and territorial epidemiologist reports, influenza activity peaked during late December, when 50 states reported local, regional, or widespread influenza activity. The peak number of states reporting regional or widespread activity during the previous 4 seasons ranged from 35 to 44.
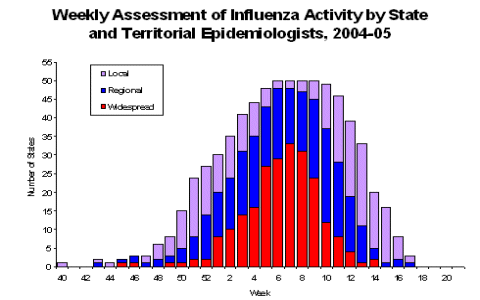
During the 2004-05 U.S. season, influenza activity occurred at low levels from October to mid-December, steadily increased during January and peaked in mid-February. Influenza activity peaked during the week ending February 19 (week 7) when 15 states reported regional influenza activity and 33 reported widespread activity. Outbreaks of avian influenza A (H5N1) among poultry continued to be reported in Southeast Asia throughout the 2004-05 season. From mid-December 2004 to June 28, 2005 these outbreaks were associated with human infections and deaths in Vietnam (60 cases and 18 deaths) and Cambodia (4 cases, all fatal).
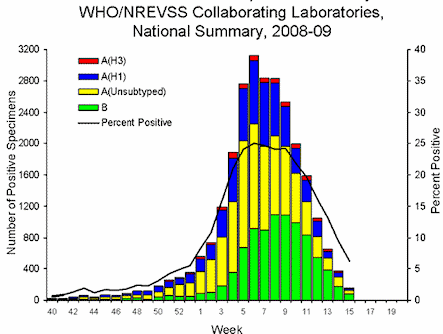
Of the influenza viruses analyzed this season, most were related to the strains included in the 2008-09 influenza vaccine. During the 2008-09 season, influenza A (H1), A (H3), and B viruses have co-circulated in the United States. Influenza A (H1) viruses have predominated during the season overall, however, the most commonly reported influenza virus has varied by week. From week 40 through week 10 (September 28, 2008 March 14, 2009) influenza A (H1) viruses were more frequently reported and from weeks 11 through 13 (March 15 April 4, 2009), more influenza B than influenza A viruses were reported. During week 14, more influenza A than influenza B viruses were reported nationally and in six of the nine surveillance regions.


