|
U.S. Department of Defense Office of the Assistant Secretary of Defense (Public Affairs) News Transcript |
| Presenter: U.S. Army, Command Surgeon, Combined Joint Task Force 82 and 82nd Airborne Division, Col. Jeffrey Johnson | February 19, 2008 |
MODERATOR (Lt Col Vician): Good morning, everyone. Our briefer today is Colonel Jeff Johnson, the command surgeon for the Combined Joint Task Force 82 and the 82nd Airborne Division. Colonel Johnson has been in Afghanistan since January of last year and has been working closely with the Afghan Ministry of Public Health to advise on and further develop Afghan health affairs.
This is Colonel Johnson's first time speaking to us from Afghanistan, and he's coming to us today from Bagram Airfield.
And with that, Colonel Johnson, I'll turn it over to you for your opening comments, sir.
COL. JOHNSON: Great. Thank you. Good morning from Bagram, Afghanistan. I'm Colonel Jeff Johnson, the command surgeon for Combined Joint Task Force 82 and Regional Command East. I'm a family physician and have served in the Army for the past 16 years. I'm responsible for the health services provided to the U.S. contingent here in Afghanistan. I also have the privilege of coordinating all of the health-related development efforts in Regional Command East.
Thank you for the opportunity to talk with you today about the incredible Afghan health sector progress that's been taking place here in the Islamic Republic of Afghanistan. The assistance of the U.S. and international forces and the nongovernmental organizations has made tremendous progress in the past 13 months and even more so since the fall of the Taliban in 2001.
The impact of medicine on stability cannot be underestimated. Health is a -- obviously is a basic need of everybody. It's a universal commodity that crosses across gender, religion, tribal affiliation and political persuasion.
The interesting thing about health that we found is that it doesn't choose sides. It doesn't try to recognize right or wrong. And that really gives us the ability to be able to leverage health care and attempt to try to create and maintain stability here in Afghanistan.
As we arrived 13 months ago here to Afghanistan, it became very clear to us that we needed to nest our efforts along with the leadership of Afghanistan and ensure that our approach was the Afghan -- (audio break) -- health care development.
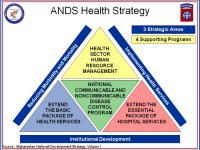
The minister of Public Health is Minister Fatimi, and he is an articulate man with a very clear vision. He has communicated his strategic plan to us all and really requested of us to leverage all of the international assets in order to be able to help create and maintain the stability here in Afghanistan. He articulated that message in the Afghanistan national development strategy, and it provides us the opportunity to engage in solutions that really present a unified national plan regardless of whether you're wearing a uniform or whether you're wearing a sports jacket or a polo shirt. The Afghan health sector strategy must be supported, from our perspective, if we're to be successful here in achieving the most health development that we can.
As we came into Afghanistan, we also noticed that there had been a lot of excellent work that had been done since the fall of the Taliban in 2001. Clearly, those efforts were targeted at the situation that existed at that time. The challenge for us was looking at where were we in 2007 and what did we need to do to adapt ourselves in order to be able to meet the requirements of the Afghan health system, as well as to support Minister Fatimi in his direction for the country.
There really were four areas that we wanted to make sure that we concentrated on and focused ourselves into in a change. The first was, we really wanted to get away from looking at short-term goals and really focus on long-term effects as the standard for where we were headed. We also wanted to make sure that we were looking at how do we build capacity in everything that we do, as this is one of the most critical elements in establishing long-term success. Furthermore, empowering the Afghans to take the lead always is a concept that we wanted to make sure that we highlighted and articulated down to the units that are actually out executing inside of Afghanistan. And finally, we wanted to make sure that we changed to have a deliberate emphasis on ensuring that we were developing the intellectual capacity of the Afghans who are here and who are executing the health-care mission inside of their country.
How are we really doing all of this? Really, we're trying to accomplish this via medical engagements and leveraging the partnerships with all of the different stakeholders that are here in Afghanistan in order to set the stage for improved health care delivery.
I'm excited to be here with you all this morning and to give you a glimpse of the progress that has been made, partnering with the Afghans over the past year. I'm happy to take some questions at this point.
MODERATOR: Thank you, Colonel Johnson, for that comprehensive overview of the operations there. When you ask your question, please remember that he cannot see you, so identify yourself.
Pauline?
Q Pauline Jelinek of the Associated Press. Colonel, could you describe the Afghan health system a little bit in statistics? How many doctors do they have? How many more do they need?
What are the greatest needs -- hospitals, clinics, that sort of thing -- just with numbers, if you have them?
COL. JOHNSON: Right. It's a good question, and to be honest with you, a little bit outside of my scope. My concentration is really here in Regional Command East.
The other piece that I think is important for us to recognize is that the way that the Afghan health sector is set up is not the same as what it would be, say, back in Kansas. It is really structured at the base with health post -- health posts are the mechanism by which they do, and there's a community health worker that works there. These are generally minimally trained health care providers that live and take care of patients inside of their homes. And that's down at the village level. That's then built, on top of that, with the basic health center, which is where you first start seeing trained physicians and nurses. And that's really your outpatient care.
Built on top of that are comprehensive health clinics, which again, usually are in villages and towns the size of about 30 (,000) to 60,000 people, and there you're you going to see some -- for the first place you're going to see x-ray, pharmacy, laboratory, and some inpatient care. Then it's very much a district and a provincial system from there on up, where you have district hospitals, provincial hospitals, and then regional hospitals that tend to see the patients as they're moving up and they're moved from one echelon up to the next.
The exact number of health care providers that are in Afghanistan -- I don't have that exact number for you, I apologize for that up front. But what we are seeing is that the access to health care here in Afghanistan is growing incredibly over the course of the last six years. Back in -- at the fall of the Taliban, the number of the population -- the percentage of the population that had access to health care at that point was 8 percent. In 2006 it was 33 percent, and today in 2008 it's up to 79 percent.
So although I can't tell you the exact numbers, I can tell you that the access to care for the average Afghan who's out there at the village level -- 80 percent of the time, they're able to get their needs met at one of those echelons of the health care system.
Q Your area -- when you talk about building capacity, is it the training of these local workers, the setting up of these local centers? What is the capacity building thing that you're doing?
COL. JOHNSON: Yeah, you're exactly right. The capacity piece is that most of these health care providers have had intermittent opportunities to train over the course of the last 10 to 15 years, as you can imagine, with some of the turmoil that was taking place before this. To be honest with you, many of the women didn't have a chance to have any kind of training at all.
So if you can imagine somebody who was originally trained 10 or 15 years ago and then was not practicing, sometimes there are some gaps, as medicine changes, as medicine evolved over the course of time.
What we found, in building this capacity, is that we need to go back in and just provide them some refresher training on top of the training that they've already had. Building capacity also just exists from a perspective of, how do they use the equipment that has been either donated, or that they've purchased, that they may not have great experience with, in being able to have had that same type of equipment when they training?
I think a good example of the capacity building is down in Ghazni city, which is in the province of Ghazni. We have one of our battalion surgeons who, on a weekly basis, conducts a medical education seminar. Originally that was done on the U.S. FOB. And the Afghans would come onto the FOB and hear a lecture on use of antibiotics, or an understanding of how to better treat hypertension, as an example.
What we've seen over the course of the past 13 months though is the Afghans again taking the lead, taking that same structure, moving it out to the provincial health director's office. And they now conduct those same capacity building, intellectual building seminars on their own -- Afghan-led, Afghan-taught. And maybe a good way to look at that is, before the Afghans were turning the slides, and the U.S. provider was giving the education. Now the Afghans are giving the education and the U.S. provider is flipping the slides for them -- to me, an incredible progress, and charting the way for them to continue to have a self-sustaining process.
MODERATOR: Courtney.
Q Hi, Colonel. This is Courtney Kube from NBC News. I have two questions for you.
First, can you give us an update on some of the specific effects that you're seeing on the health in RC East, because of the bitter cold weather that you're having this winter there?
And then also, on the issue of internally displaced persons or refugees, we know that RC East saw quite a bit of violence in 2007. Do you have any estimate of how many refugees are in the area? And how specifically are the coalition, the Afghan government, how are they accounting for the health care of those persons?
COL. JOHNSON: Sure. Let me do the last piece here first, and then I'm probably going to have you repeat the first question.
With regard to the refugees, to be honest with you, I think there's a good news story here. If we look at the refugees that came across the border from Pakistan into Khost province, that was really a response to some of the turmoil that was taking place in Pakistan. And the people there understood that their lives potentially could be better if they were in Afghanistan, going to the health clinics, getting their health services accomplished inside of Afghanistan.
There were about somewhere -- a rough average -- about 10,000 people that moved across the border and integrated into the health care system that existed in the provinces of Khost and it spilled it over into Paktia as well. It's very interesting from our perspective, because, again, the Afghans have the lead -- Minister Fatimi's direction has the lead here. They were able to take care of almost all of the needs of those refugees that came across the border over the last couple of months.
We see ourselves, from the U.S. military standpoint, as really being the third line agent where assistance would come from. That second line agent is the United Nations, and UNHCR does a wonderful job at managing populations that are displaced inside of the country here.
It was interesting that formally we were not given any requests from the minister of Public Health in that he needed additional assistance from the U.S. military. And I think that's a great news story showing how the minister of Public Health, his assets, his responses were able to, for the most part, meet the needs of those displaced persons as they moved across the border.
If you could repeat that first question again, I'd be glad to answer that for you.
Q Sir, I was just asking about this -- any specific effects you've seen on the health in RC-East or even in the rest of the country because of the bitterly cold weather that you've experienced. Specifically, have there been any instances of disease outbreak, flu?
COL. JOHNSON: Right. I got the question now.
Fortunately, inside of Regional Command East, the winter here has been fairly cold, but the snows have not been as much as what they have been in some of the other years. Most of the bitter cold has been out in Regional Command West, and that's where they have had the most difficulties.
Again, Minister Fatimi and his deputies have been working diligently at meeting the needs of the people, delivering humanitarian aid packages mostly consisting of things like charcoal, blankets, heating oil and food products. But to be honest with you, for where most of this is taking place out in RC West, that's coming through the minister, as well as with some coordination with the International Security Assistance Forces, ISAF, who has the responsibility for RC West.
Here, specifically inside of RC East, we have not seen an increase in disease outbreaks. And the people, to be honest, are a little bit hardier here because they normally live in the mountains and they have rough winters. They prepare for that and have done really quite well here this summer -- I'm sorry -- this winter with the temperatures that have been here.
MODERATOR: Al?
Q Hello, Colonel. It's Al Pessin from Voice of America. Can we shift focus for a second to the U.S. troops? As you know, there are a lot of issues up about the -- especially the mental health of the troops. Can you tell me what you're seeing and what you're doing to address some of the issues we hear about, such as PTSD and increased suicide rates, partly based, at least, on long-term multiple deployments?
COL. JOHNSON: Yes, sure. I don't want to get too far off-track here, in that the purpose is, we're trying to describe the development of the Afghan health sector and how we've been doing that. Obviously, we are taking a very close look at our U.S. population as well, engaging in the screening of these soldiers prior to them leaving theater; making sure, as we're an airborne unit, that prior to them resuming airborne operations, that they get screened not only for mild traumatic brain injury but also for PTSD. And we feel like we have a pretty good handle on that.
But I think it's interesting, as well, that just as we have the same interest in the mental health of our U.S. troops, that is one of the initiatives of Minister Fatimi as well, and the Afghan health care system.
They are looking aggressively at trying to make sure that they address mental health issues which really have been forgotten here in Afghanistan. If you can imagine a group -- a generation -- a couple of generations that have seen the horrors of war over and over again, you can imagine how that has even magnified in their people. And that's been a place where our social workers, our psychologists, our psychiatrists have been able to partner, along with the Afghan system, again, building their intellectual capacity, what are the most modern ways of treating depression, post-traumatic stress disorder in the Afghan people as well. And we've seen some great movements forward in assisting them with that approach as well.
Q Colonel, aside from the screening, do you have mental health care initiatives for the troops? Do you have enough mental health care providers to deal with the issues you have to deal with?
COL. JOHNSON: Yeah, right. We certainly have, in my estimate, the minimal necessary required mental health providers required to accomplish the mission here. We have taken a very close look and looked at the challenges of where we have troops that are in frequent contact and actually moved mental health assets out forward in order to be able to take care of them in proximity to that location. The process by which they're receiving care here is world class, having the right medications, the right ability to be able to give them therapy, as it might need be, and tailored to be able to meet the condition that they have and the environment that they're in.
That being said, even with the requirement to be able to provide mental health care to our troops, we still have the ability to be able to have those same mental health assets working with the Afghans, teaming with them in order to be able to find out what are the needs of those local communities that are seeing the same -- the same difficulties and having the same issues with the inside of the Afghan system.
Q I'm sorry, just real quickly, When you say you have the minimum required, it sounds like you're saying you could use some more.
COL. JOHNSON: I would completely disagree with your assessment of that.
The minimum requirement is exactly what we need. I am not looking to have any additional mental health assets in order to be able to meet the requirements that we have here.
I think one of the things that the people of Afghanistan have really taught me this past year is that we need to be very frugal with our assets, and we need to determine what is the minimum required amount to be able to meet the mission and to be able to get accomplished what needs to be done. And that's exactly what I'm referring to, is we have just the right amount of mental health providers that are here to meet the requirements that are needed.
Q Thank you.
Q Colonel, it's Meredith MacKenzie with Talk Radio News Service. You talked about developing the intellectual capacity. What's the state of medical schools in Afghanistan, and how are you training the next generation of medical professionals?
COL. JOHNSON: Yeah, it's a great question and a little bit outside of my scope. It's interesting how the different ministries are set up here in Afghanistan -- a little bit different than they are back in the United States. The minister of public health has under his responsibility the requirement to provide the health care for the people. The education for the physicians and for the allied health care providers falls under a different ministry which I don't have as much contact with. But I can tell you that the medical school that was a thriving medical school in the 1970s in Kabul, that was really dismantled during the '80s and the '90s, has been re-established now, and they are working towards graduating their first class of doctors to come out since the fall of the Taliban.
Understand that to produce a physician, it's more than a one-year process to do that, and you're typically talking about a six- to seven-year lag time in order to be able to get those doctors coming out again. And so when we talked about building intellectual capacity, we understand that there's the piece that's being built inside of the medical schools and how those doctors are being trained, but we've also understood that we really have to put an emphasis on connecting with the health care providers that are already out in the communities, and making sure that we don't disenfranchise them from their ability to be able to continue to work and provide excellent health care.
Q What kind of training regimen, for those people who work, and you said the village level; you said more of a minimal sort of health care provider that goes to houses. Where are they trained, if not in medical schools?
COL. JOHNSON: Right.
The health care workers that are down at the health posts -- typically it's apprentice-style training that they got. The formal education typically is not there. To be honest with you, that is a piece of the Afghan health care system that we have not engaged with extensively, just in that where we want to concentrate our efforts is on that first echelon, where the trained health care providers exist, where those midwives exist. And that's really where we've spent most of our effort.
The process by which we do that is really doing a lot of intern- style work with them, where we will go to their clinics or to their hospitals. And we sit down at the table with them, and as they're seeing patients, typically through an interpreter, understanding what the problem is, and then discussing that patient problem, what the treatment plan is going to be, how the diagnosis is made, and discussing that whole process with the Afghan health care provider, and really doing a one-on-one education process with them, is what we've found to be the most effective, once you're down at the village level, at the township level.
We have not engaged extensively inside of their formal schools. There are excellent non-governmental organizations that are doing that, as well as other intra-agency partners that are working those avenues. Where we really see our niche is being able to get into those communities, be able to work one on one, sharing experiences, our medics to their health care providers, our doctors to their doctor, in improving their ability to deliver health care at that level.
MODERATOR: Jeff.
Q Colonel, Jeff Schogol with Stars and Stripes.
Are the Taliban targeting any midwives, or doctors who are women, that you are training?
COL. JOHNSON: Yeah.
You bring up an interesting question. And I would say that it applies not just to women, but we've seen it apply to men as well. I think it is reasonable for us to say that there is a deliberate action by the Taliban in many instances to look at, who are those health care providers that are willing to work along with the coalition forces that are here, and trying to influence them from their Taliban perspective.
What we have really been able to do, though, is work hand in hand along with the operations folks here, so that as they move into areas that have a very strong Taliban influence and begin to separate the people from the Taliban, that we are then able to move in right behind and begin to work these partnership relations in that one-on-one activity. Obviously, it implies that there is a lasting presence once the Taliban is cleared out of an area, and that is something that -- I have been very amazed that the Afghan National Army and the Afghan National Police have provided that continuous presence inside of these areas that we are able to move in, clear the people away, separate them and then be able to bring back basic services to them. And for us, specifically, it applies to health.
Q Is there are a murder and intimidation campaign against doctors and other medical care providers, specifically women?
COL. JOHNSON: Right. I think it's a good question, and I can't necessarily get too much into the detailed pieces of that security aspect. But it is clear that the Taliban would wish to intimidate the doctors and women who are providing health care to the people. Obviously, the provision of health is something that the people see that is directly tied back into the government. And if ensuring that there's a connection between the government and the people is a formula for success and a formula for progress here, obviously the Taliban want to disrupt that.
So I would say that your statement is correct in that there are attempts at intimidation, but I think what I've also seen is some very heroic Afghans who are willing to stand up and say: "Enough is enough. It's now time for us to take our country back. It's now time for us to be able to understand what it is that our local people want, what they need and we're willing to take some risks" -- this is the Afghan health care providers -- "we're willing to take some risk in order to make sure that we can reestablish the basic needs for our people."
And from a perspective of an American who -- our lives are not every day associated with risk, that is incredibly inspirational, to me.
MODERATOR: Well, Colonel, we have reached the end of our appointment with you today. Before we close, though, I'll turn it back to you for some closing comments.
COL. JOHNSON: Great. I appreciate everybody's time here, and thank you for your questions and attention.
As you can see, I have a passion for the Afghan people and their positive future. I definitely have the opportunity now for the last 13 months to be able to see there is a positive future here. Allowing the Afghans to chart their own future and seeing their efforts to bring this to fruition is very inspirational, I think, from all perspectives.
The members of the Combined Joint Task Force 82 have had the opportunity for the past 13 months to participate in this effort. We have learned a great deal from our stakeholders, who have that common purpose in mind with us. But even more so, I'm impressed by the dedication and the heroicism of many of the Afghans who are willing to put their lines -- their lives at stake in order to be able to improve their own health care system.
As the Afghans take the lead and we purposefully put ourselves into a supporting role, we continue to see incredible progress that is, importantly, culturally appropriate, fiscally responsible and really long-term-focused.
There's undoubtedly much work that still has to be done here in Afghanistan. We have a long ways to go yet. But there is a(n) irreversible momentum that is in place. Focusing on the human intellectual development, capacity-building and the empowerment of the Afghan health sector is critical to the development here.
Also critical is the collaborative work with all of the other partners that remain essential to leveraging their synergistic skills and resources, as well as ensuring that the expertise that is there allows the Afghans to lead their international approach to their future.
We all have reason to be proud of how we've completed this task, from both the U.S. forces' perspective, as well as the interagency organizations', and we have taken heed to this challenge.
And there's been an incredible amount of courage and selfless service that's existed here in Afghanistan over the last 13 months. Afghanistan has moved one step closer, in my opinion, to being an independent, self-sufficient nation, improving health to contribute to the economic and social development, thereby leading to their own stability.
Once again, I appreciate your time today and thank you very much.
MODERATOR: Yes.
Thank you for making a house call at the Pentagon Press Corps today, and I trust that your transition over the next several weeks and your return home will go well. Thank you, sir.
COL. JOHNSON: Thank you.
http://www.defenselink.mil/Transcripts/Transcript.aspx?TranscriptID=4148
|
NEWSLETTER
|
| Join the GlobalSecurity.org mailing list |
|
|
|