Appendix C
DECONTAMINATION TACTICS, TECHNIQUES, AND PROCEDURES
1. Background
The purpose of this appendix is to familiarize DOD personnel with the decontamination procedures that may be encountered when responding to incidents that are associated with NBC-related situations. It addresses guidance on the use of TTP to support the decontamination process for both military and civilian response organizations. DOD personnel must be aware of decontamination planning and operational considerations in order to operate effectively with civilian counterparts.
2. General
The aim of decontamination is to rapidly and effectively render contamination harmless or remove it. The ability to function in a contaminated environment and perform decontamination actions is one of the factors that can reduce the effect of an attack. The goal of decontamination remains the same whether it is performed in wartime or in a peacetime response operation—to limit the spread of the contamination and reduce levels to the greatest extent possible. The tasks performed do not change, but the procedures may vary depending on the nature of the accident/incident and available equipment. Standard DOD decontamination procedures, used in an NBC environment, can be modified to work effectively in specific incident-related situations. When tasked to support a decontamination mission, reduction and containment should always be the primary focus of the operation.
3. Decontamination Basic Concepts
a. Priorities. The incident commander establishes decontamination priorities. Decontamination of exposed personnel and casualties are usually the top priority followed by equipment, facilities, and areas. NBC contamination threatening to create a downwind hazard will also have a high priority, and contamination-reduction and containment actions must begin as soon as possible.
b. Methods. All decontamination is based on one or more of the following principles: destroy toxic agents by chemically modifying them (destruction); physically remove agents by absorption, washing, or evaporation; and/or physically isolate the agent so that it causes no damage (shielding/containment). Initial efforts should focus on terminating the contamination release if responders are able to identify the source of the contamination.
c. Decontaminants. The decontaminant of choice will depend on factors like the type of contamination and the operational environment. The decontamination plan (as prepared by the incident commander's staff) will outline details such as the type and amount of decontaminant that will be used. For example, weathering is one method of decontamination; however, it may not be an acceptable alternative at an incident site due to time constraints.
4. Decontamination Planning
a. The decontamination process (as directed and coordinated through the IMS process) should be directed toward confinement of the contaminant within the hot zone and the decontamination corridor. The potential effects of the decontamination process on responder personnel are considered when developing the decontamination plan, and countermeasures such as adequate work/rest cycles are addressed.
b. The determination of proper decontamination methods and procedures are considered before the incident as part of the overall preincident planning, hazard, and risk evaluation process. No entry into the hot zone should be permitted until appropriate decontamination methods are determined and established.
c. During the course of decontamination planning, the basic steps of mass personnel decon (emergency procedures) and estimating the total number of personnel to be decontaminated will influence the amount of resources used to support the operation. These basic steps include:
Clothing decontamination and removal.
Showering (may be as simple as spraying down with fire hoses/using soap and water).
Monitoring (and medical treatment) for contamination.
Performing triage and treatment as required.
5. Personnel and Casualty Decontamination-Station Overview
a. Personnel decontamination requires a step-by-step process to reduce the contamination on casualties and personnel to a safe level and to prevent the transfer of contamination outside the containment area. The procedures used are based on a field analysis of the hazard and risks involved. This consists of checking technical reference sources to determine the general hazards such as flammability and toxicity, and then evaluating the relative risks (i.e., vapor versus liquid; blister versus nerve; radiological versus chemical and/or biological) associated with the contaminants.
b. The formal decontamination process begins in the warm zone (see Figure C-1) (contamination-reduction corridor). A controlled entry point marks the entrance to the decontamination corridor and a controlled exit point marks the exit to the cold line (a transition point between the warm and cold zones).
Figure C-1. Establishment of Safety Zones at a Hazardous-Materials Incident Scene
c. Once personnel cross the cold line, medical teams will perform triage and conduct monitoring and treatment for any injuries. Next, personnel will then be redressed/covered, moved to a holding area, and monitored for ongoing signs and symptoms of exposure. When medical triage dictates, the casualty will be treated for injuries and evacuated to a medical facility.
d. Figure C-2 depicts a sample of a personnel decontamination station that could be used to decontaminate personnel. The decontamination line may be two stations or eight stations. The basic goal is to eliminate the contaminant in a safe and appropriate manner. Each position should be manned by trained and properly equipped individuals to direct personnel and assist them, as necessary, in the decontamination process.
Figure C-2. Sample of a Personnel Decontamination-Station Layout
6. Contamination-Reduction Considerations (Personnel Decontamination-Station Operations)
a. Contamination reduction removes, rinses off, or dilutes the contaminants. This consists of three main steps, although several intermediate steps may be necessary (which will add additional wash and rinse stations to the decontamination line). The type of hazard will dictate what decontaminants are used and the best method of decontamination. The decontamination line generally consists of a primary decontamination to remove the majority of the hazard, a secondary decontamination tailored to the specific hazard, a monitor point to ensure that all contamination has been removed from the outer garment, a PPE and personal-clothing removal, and a medical evaluation.
b. Consideration must also be given to the staffing and safety of the decontamination team. The decontamination team should be fully trained on all PPE worn, as well as trained and certified on all equipment that is being operated. Decontamination team members will be dressed in Level A through Level D individual protection based on their proximity to the hot zone and the level of contamination they are expected to encounter throughout the decontamination site. All decontamination personnel, to include the equipment they used, must be decontaminated before leaving the contamination-reduction zone (CRZ). There are many approaches to decontamination, but all are built around the basic principle of contamination reduction. The hazard encountered in the mission will dictate the necessary details, but the overall process remains the same.
7. Decontamination Procedures (Entry Point) (See Figure C-2)
a. The controlled entry point is a clearly designated place at the hot line that identifies the beginning of the decontamination corridor (CRZ). The purpose of the controlled entry point is to ensure that all personnel leaving the hot zone process through the decontamination line, thereby controlling the spread of contamination. At the controlled entry point, two separate stations are set up—the equipment drop point and an emergency-decontamination area.
b. Primary decontamination can be accomplished in several ways depending on the hazard. Typically, it consists of a "wet decontamination" (i.e., emergency decon) where the individual is flushed with water to remove or dilute the contaminants. A "dry decontamination," such as brushing and scraping, can be another alternative for other contamination removal (i.e., radioactive-contaminated physical particles). Other considerations such as the hazard's reactivity with water and its solubility will be factors in determining the decontamination method. Once the primary decontamination has been accomplished, the individual moves to the secondary decontamination.
c. Primary decontamination activity at the equipment drop may consist of a tarp or table where all equipment used in the hot zone is placed. The equipment drop serves a dual purpose. First, it ensures that all potentially contaminated equipment stays within the contaminated area, and secondly, it allows the equipment to be reused by anyone reentering the hot zone. This will minimize the amount of equipment brought into the hot zone that will later require decontamination or disposal.
d. Secondary decontamination can consist of one to several stations depending on the hazard. The decontamination team must be available to supervise the operation and assist in the processing of personnel. The team is trained to help the personnel decontaminate their outer clothing from top to bottom (always moving the contaminates toward the ground). To control the spread of contaminants, low-pressure water should be used and overspraying and splashing should be kept to a minimum. The decontamination site should be established in an area where contaminated runoff can be controlled.
e. Once the primary and secondary decontaminations are complete, the personnel should be monitored for any residual contamination. If the hazard is known, monitors such as the chemical-agent monitor (CAM), radiacmeters, and commercial instruments can be used to perform this function. When working with an unknown substance or without monitoring devices, use visual observation. Stains or discoloration of the PPE should be noted as well as any obvious signs and symptoms that the personnel exhibit indicating exposure to the hazard. If the contamination is still present (visually observed or detected by monitoring devices), the personnel return to the primary and secondary decontamination areas to repeat the procedure, paying specific attention to the areas noted by detection devices. After the contamination check, the outside of the PPE (i.e., Level A suit) should be decontaminated (however, personnel should not touch the PPE with their bare hands).
f. The decontamination and monitoring process is unique to each accident/incident. Decontamination techniques may be both physical and chemical. The decontamination methods selected should be tailored to the hazard, responders on scene, location, and equipment available. The equipment and the response units' knowledge, as well as the IC's operations section technical knowledge and research will be of assistance when dealing with hazards. Whichever method(s) is used, the outcome should be the elimination or reduction of contamination to a safe level while confining the hazard to the hot zone and decontamination corridor.
8. Decontamination Procedures (SCBA Removal) (See Figure C-2)
a. As the personnel enter this station, the decontamination team unzips and peels back the personal protective suit, exposing the SCBA. The decontamination team should not touch any part of the inside of the suit and the individual should not be touched by any part of the contaminated side of the suit. At this point, the individual can begin removing his PPE or conduct an air-bottle exchange and return to the hot zone. If monitoring devices are not being used or the hazard is unknown, the order of the next two stations may be reversed to protect the respiratory system of the individual until all outer garments have been removed.
b. If the individual is returning to the hot zone, the air bottle or the SCBA will be changed with the assistance of the decontamination team members. At this station, depending on the risk of exposure, the air bottle and SCBA can be removed and exchanged for clean, serviceable ones. Off to the side of this station, another team would replace the air bottle or SCBA and then reseal the individual's suit. The individual can then reenter the hot zone to continue operations.
c. Individuals continuing through the decontamination process will remove their own facepiece and loosen the straps on the SCBA. The decontamination team assists in removing the SCBA and places it in a collection container off to the side. The individual then continues on to the next station to the conduct PPE removal.
9. Decontamination Procedures (Showers) (See Figure C-2)
Procedures conducted at this station can occur on site using portable enclosures if contamination of personal clothes is suspected. Portable enclosures usually have three areas—one for the removal of clothing, another for showering, and a third for donning clean clothes. Clothing that is removed should be bagged and labeled for each individual, in case uncontaminated clothing can be salvaged. The individual should shower, using generous amounts of soap and water and scrubbing downward from head to toe. After the shower, the individual moves on to the next area to dress in clean clothing. Clothing such as cotton coveralls or hospital scrubs may be used for individuals when other clean clothes are not available. The individual exits the showering facility into the cold zone (contamination-free zone). All cleaning items used during the decontamination process should be bagged for disposal, and decontamination runoff is controlled to limit the spread of contamination. Another factor to be considered at this station should be the environmental effects on personnel. During cold weather, appropriate measures are taken to eliminate the possibility of individuals receiving cold-weather injuries.
10. Decontamination Procedures (Medical Evaluation) (See Figure C-2)
After completing a thorough decontamination, individuals should proceed to a medical evaluation station. The individuals' vital signs are taken, documented, and compared with the baseline information taken before entering the hot zone. Any individual showing any signs or symptoms from exposure or injury should be transported to a hospital for appropriate treatment and monitored after ensuring that they have been decontaminated as completely as possible. Proper documentation on all individuals processed through the decontamination corridor must be maintained. The names of individuals, methods of decontamination, and any exposures or injuries should be included. Once the individuals leave the medical-evaluation area, the decontamination process is finished.
11. Casualty Decontamination
For more detailed information on casualty decontamination procedures, see applicable service documents such as FM 8-10-7.
a. The casualty decontamination process discussed in this manual (see paragraphs 12-18) is similar to those discussed in applicable service manuals. The procedures described in this appendix were modified, where necessary, to account for large numbers of casualties, casualties without protective equipment, and responders wearing the PPE that conforms to OSHA standards.
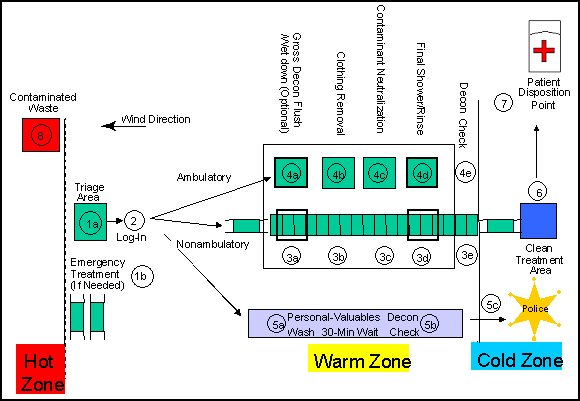
b. Casualty Decontamination Stations (see Figure C-3). Casualty decontamination is time constrained. The layout of the decontamination corridor is depicted in Figure C-3. The layout of the stations within the decontamination corridor should be set up to process unprotected causalities as quickly as possible. The decontamination corridor begins at the hot line and extends through the warm zone with the clean treatment and patient disposition area 30 to 50 meters into the cold zone. Casualty decontamination should be established in an area where the runoff could be controlled. The personnel (responder) decontamination corridor should not be visible from the casualty decontamination corridor. This should prevent the perception that individuals in protective gear are being processed through the decontamination corridor and receiving treatment before casualties. Overall, the emphasis of casualty decontamination is the quick removal of contamination to reduce or prevent further personal injury and prevent the spread of contamination.
Figure C-3. Sample of a Casualty Decontamination-Corridor Layout
c. In the decontamination process, equipment decontamination solutions are not used on the skin. These solutions may cause burns and further injury. Mild, nonabrasive soaps or a chlorine solution should be used. When using chlorine solutions, prepare two separate concentrations. A 0.5 percent chlorine solution should be used to decontaminate the patient's skin and splints and irrigate wounds. A 5 percent solution should be used to decontaminate gloves, aprons, litters, and cutting devices. (A 0.5 percent solution can be created by adding 2 quarts of household bleach to 5 gallons of water. A 5 percent solution is approximately the same as household bleach; there is no need to dilute.) When removing gross contamination from the patient's skin before the first rinse, the M291 kit can be used.
12. Casualty Decontamination (Triage Point) (See Figure C-3)
a. As personnel arrive at the triage station, symptomatic personnel should be separated from personnel not displaying symptoms. A quick medical assessment is performed to determine the medical status of each individual and the decontamination station the individual will proceed to. The order in which personnel are processed through decontamination is based upon their triage status and the instructions of the medical official in charge. If a respiratory hazard is present, individuals awaiting triage and decontamination should be provided with respiratory protection. Ambulatory casualties will be processed separately from the nonambulatory (litter) casualties.
b. Communicating as much information to the casualties as possible will foster cooperation from those waiting to be decontaminated. Before being processed through the decontamination stations, casualties requiring emergency life-saving medical treatment are routed to a medical-treatment station collocated with the triage point. When dealing with large numbers of casualties, many of the less severely injured walking wounded may be required to wait. Casualties being monitored following decontamination should be placed in designated rest areas located in the cold zone.
13. Casualty Decontamination (Emergency-Treatment Area) (See Figure C-3)
Medical personnel at this station provide life-saving emergency medical care only. The amount of medical treatment given should be minimal in the contaminated treatment area. Airway management, cervical immobilization, bleeding control, and treatment with nerve-agent antidote kits are all measures that could be performed to stabilize the casualty and increase his survivability throughout the decontamination process. Once the casualty is stabilized, he should be processed through decontamination as a nonambulatory patient and receive further medical care in the clean area. Bandaging of nonbleeding wounds may be postponed, based upon the overall casualty load and the severity of wounds, until the casualty reaches the clean treatment area. This permits wounds to be fully decontaminated before being passed through to the clean treatment area.
14. Casualty Decontamination (Nonambulatory Decontamination) (See Figure C-3)
a. Litter casualties will require timely decontamination. At the triage station, all nonambulatory casualties are placed on a litter and brought to the nonambulatory decontamination area. The litter is placed on supports in order to keep the casualty raised above the ground. Process the casualty through headfirst to ensure that the airway (i.e., the head) is upwind if possible.
b. If biological or radiological contamination is suspected, the casualty's clothes should be wetted before attempting removal to prevent the reaerosolizing of the hazard. Casualties wearing respiratory protection should keep the facepiece on until after being monitored and confirmed clean, unless it interferes with the establishment of an adequate airway.
c. If it is necessary to decontaminate the casualty's face, perform the procedure without exposing him to vapor hazards. To accomplish this, the casualty should hold his breath and close his eyes while the protective mask is removed and the face and facepiece are decontaminated. When decontaminating a casualty without respiratory protection, decontaminate him headfirst, wet him down if required, cut away and remove all his clothing, decontaminate the front and back sides of his body with a 0.5 percent chlorine solution, conduct a final wash or rinse, and then check him. If a litter is used, always decontaminate it as one would decontaminate the casualty and change the litter after removing the casualty's clothing and when transferring him to the cold zone.
d. If the casualty is unable to accomplish this procedure, the decontamination team should postpone decontamination of his face until removal of the facepiece is accomplished at the shuffle pit located on the cold line. Instead, the decontamination team should decontaminate the outside of the facepiece with a 0.5 percent chlorine solution and cut away his outer clothes, being careful not to disturb holes or stained areas that might provide evidence in a criminal prosecution.
e. The decontamination team should ensure that the cutting device and their gloves and aprons are rinsed with a 5 percent chlorine solution before coming in contact with the casualty. The casualty's clothes should be bagged and sealed separate from his valuables. Both bags should be labeled with the casualty's name and placed into a closed container off to the side for evaluation and decontamination at a later time. After all clothing is cut away, the casualty is transferred to a clean litter.
f. Before washing the casualty, gently brush or blot all visible contamination to reduce the chance of the hazard reacting with water. When all visible contamination is removed, the casualty should be washed with soap or a 0.5 percent chlorine solution and copious amounts of water. The extent of washing and the time spent decontaminating will depend on the hazard and the casualty's exposure.
g. Casualties whose skin have come in contact with a hazard will require more extensive decontamination than those exposed to vapors only. When the extent of contamination is uncertain, the decontamination team should always assume a worse-case scenario. The decontamination team should begin the decontamination process at the patient's head and face, allow no blockage of the airway, and be careful not to flush contaminants into the casualty's eyes or wounds. Medical personnel should remove all contaminated bandages and wash and rinse wounds from the center outward. Following the washing and rinsing of wounds, cover them with water occlusive dressings or plastic wrap to prevent secondary contamination. Splints should be decontaminated in place by applying a 0.5 percent chlorine solution to the splint, padding, and cravats. If the casualty's eyes are contaminated, flush them with a normal saline solution. When all wounds are cleaned and dressed, the remainder of the casualty's body will be decontaminated. During the decontamination process, pay special attention to the hair, nails, skin folds, joints, and ear and nose cavities. Rinse the casualty with large quantities of low-pressure water. If the casualty has a triage tag, drop it into a plastic bag, seal the bag, and rinse the outside of the bag with a 5 percent chlorine solution. The triage tag can now accompany the casualty. Medical personnel will write a new triage tag when the casualty reaches the clean treatment area. Once the triage tag is copied, the original tag (still sealed) is considered contaminated and should be set aside to be disposed of with other HAZMATs during the recovery phase.
h. When the casualty is fully decontaminated, he is moved to the next area to be monitored for completeness of decontamination. Monitoring can be done by a variety of methods. M8 paper, CAM, low-level radiacmeters, and commercial devices can all be used for the appropriate hazard. For unknown hazards, visual inspection may be the only method available for checking the thoroughness of the decontamination process. When monitoring instruments are used, ensure that the area in which the casualty will be monitored is free from contamination. If the casualty is still contaminated, he will be moved back to the wash area and the decontamination process will be repeated. Casualties that are monitored and determined to be free of contamination will be moved to the clean side via the shuffle pit.
i. The decontamination team carries the casualty by litter into the shuffle pit and places the litter on supports. After rinsing their gloves and aprons with a 5 percent chlorine solution, the decontamination team lifts the casualty from the litter and removes it. The decontamination team on the clean side of the cold line will provide a clean litter for the casualty. The decontamination team from the warm zone will remove any respiratory protection still on the casualty and decontaminate his face with a 0.5 percent chlorine solution. The facepiece returns to the warm zone to be decontaminated at a later time. All equipment and personnel involved in operations in the warm zone must remain there until they are fully decontaminated. The decontamination team from the clean side of the cold zone carries the casualty by litter out of the shuffle pit to the clean treatment area. Upon reaching the cold zone, the casualty (still on the litter) should be covered to prevent hypothermia.
15. Casualty Decontamination (Ambulatory Decontamination) (See Figure C-3)
a. Casualties who are able to walk and assist in the decontamination process are sent to the ambulatory decontamination area. This includes casualties who have minor injuries and minimum exposures that have received the proper treatment. Casualties are processed in order by triage status; some casualties may be routed to a holding area to await decontamination. This is especially true in accidents/incidents with large numbers of-walking-wounded casualties. Symptomatic casualties are processed before casualties that are asymptomatic (personnel not showing symptoms).
b. Gross decontamination is performed first. This consists of removing any visible contamination from the casualty. If radiological or biological contamination is suspected, the casualty's clothes should be wet down before and during the removal process. The casualty's valuables should be bagged, sealed, and labeled with his name. Casualties wearing respiratory protection should be assisted by the decontamination team in decontaminating their faces and replacing their facepieces without further exposing them to vapor hazards. If this is not possible, postpone decontamination of the face until the facepiece is removed at the end of decontamination. Triage tags should be placed in a plastic bag, sealed, and rinsed with a 5 percent chlorine solution. The triage tag accompanies the casualty until it is rewritten in the clean treatment area. The triage tags (still sealed) should be collected in a plastic bag then returned to the warm zone to be disposed of with other hazardous waste. Casualties are then separated, sending male patients to one corridor and female patients to another. The disposition of families and small children should be considered when establishing the decontamination corridors. Throughout the decontamination process, casualties should be shielded from bystander and media viewing.
c. In the appropriate decontamination corridor, the casualty should be assisted in removing all outer clothing down to his undergarments. Clothing should be bagged, sealed, and labeled with the casualty's name, then placed into sealed containers for inspection at a later time. If biological or radiological contamination is suspected, continue wetting the casualty's clothing during removal to prevent the reaerosolizing of the agent. Cut away the casualty's clothing. Keep the clothes from contacting the casualty's face during removal. After clothing removal, apply a decontaminant to the casualty or have him shower with soapy water, as appropriate. After the decontaminant application, the casualty washes and rinses thoroughly, starting at the head and working down to the feet. He should pay special attention to his hair, nails, skin folds, and ear and nose cavities. Soap or a 0.5 percent chlorine solution should be used, if available. The decontamination process should not be delayed due to a lack of soap. Use large amounts of water.
d. After washing and rinsing thoroughly, the casualty moves on to the monitoring area. The casualty is monitored from head to toe for completeness of decontamination. If any residual contamination is found, return the casualty to the shower to repeat the decontamination process. Casualties who are monitored and contamination is not found should have their respiratory protection removed, if it is still present. If decontamination of the face was postponed, it should be done with a sponge soaked in a 0.5 percent chlorine solution upon removal of the facepiece. Provide the casualty with a cover (sheets, coveralls, hospital gowns) and direct him to the clean treatment area in the cold zone for further medical assessment.
16. Casualty Decontamination (Clean Treatment Area) (See Figure C-3)
a. Upon completion of decontamination, both ambulatory and nonambulatory casualties are brought to the clean treatment area in the cold zone for triage and medical evaluation. The clean treatment area should be located at least 30 to 50 yards from the cold line. Monitoring devices should be placed between the cold line and the clean treatment area to detect any drift of hazardous vapors from the warm zone. If the casualties have been previously triaged, the decontamination team will fill out a new triage tag updating it as necessary. The triage tags brought through the decontamination process in sealed bags are considered to be hazardous waste and must be disposed of properly. If triage has not been done, a triage tag is filled out as medical personnel perform secondary assessments on each casualty. All life-threatening injuries should have been identified, decontaminated, and stabilized, and casualties should have received priority on transport upon reaching the cold zone.
b. Based on their triage status, casualties are moved into selected treatment areas. Casualties in the treatment areas will need protection from observation by the media and may need protection from the weather. Blankets, hospital gowns, or some type of cover should be provided during the casualties' wait for transportation. The most critical casualties will receive advanced care and be prepared for transportation first. Casualties who have been identified as requiring a lesser degree of medical care will receive first aid while awaiting transport to a medical facility. All casualties should be transported for medical evaluation regardless of injuries or symptoms.
17. Casualty Decontamination (Casualty Disposition Point) (See Figure C-3)
a. As transportation to a medical facility becomes available, the casualty is moved to the transportation disposition point. One dispatcher in this area should handle all coordination with medical facilities to prevent the overloading of one hospital. Casualties with the most critical injuries are transported first. The walking-wounded casualties and casualties without injuries or symptoms can be transported by means of buses or vans. Vehicles used to transport patients should have all surfaces, benches, and exposed areas covered by plastic sheeting. Under ideal circumstances, patients should be fully decontaminated on scene. Planning and coordination must include the preparation for casualties who leave the scene and refer themselves to a medical-treatment facility.
b. All personnel handling patients in the cold zone or transporting them should wear appropriate levels of PPE. Any patients being transported by air should receive extra attention to ensure that they are fully decontaminated before being placed aboard the aircraft. Hazardous vapors released into a confined space could have detrimental effects on the unprotected pilots and crew. Information on all patients should be recorded for accountability. Any information that will help track patients should be included in the accountability record, such as the patient's identification; the type of contamination; the extent of injuries; and where, when, and how the patient was transported. The decontamination process will continue until all persons exposed to the agent are received at the medical facilities.
18. Casualty Decontamination (General Patient Decontamination Considerations)
a. The decontamination team must wear the PPE and the respiratory protection that are required for the hazard. The decontamination team at the triage point should have the highest amount of protection needed for the hazard. As patients move through the decontamination line, liquid and vapor hazards are reduced. This allows personnel closer to the cold line to wear a lower level of protection than the decontamination team at the triage station near the hot line. Contact with the patients should be minimized to limit contamination transfer. Medical and decontamination teams should monitor each other for signs and symptoms of agent exposure.
b. Use warm water in cold weather to provide patient comfort and reduce the chance of patient hypothermia. If warm water is unavailable, cold water may be used but weather conditions must be considered. Decontamination may have to be accomplished indoors to prevent patient exposure and cold-weather injuries. School gyms and other facilities containing showers are possible locations for decontamination stations. Minimize the spread of contamination by covering the interior of patient transportation modes with plastic sheeting and promptly bagging all contaminated items as they are removed from the patients.
|
NEWSLETTER
|
| Join the GlobalSecurity.org mailing list |
|
|
|